Eight Things I Learned at NatCon 22
Introduction
NatCon 22 was a time to redefine mental health in a new way. We saw old friends, colleagues, and people, lots of people. We thought of the people we lost and the heroes we were among, The clinicians that gave of themselves to meet the needs of each other and their clients—the shift to telehealth overnight when clinics could no longer see clients in person. They met on driveways, in parks, wherever they could to keep care moving forward, to redefine mental health care.
Overview
We have to use the lessons learned during the pandemic to increase access to care, quality of care, and the value of care. I remember eight things I learned while at NatCon22, including CCBHC, outcome measures, value-based payments, and a few other things. But first, we have to play video games and dance, and I am not kidding.
1. Video Games
So about the video games. Payers figured out that they had to think outside the box to reach young people. They did not exactly do that; actually, they thought within the box or, in this case, the video game to reach their audience. They sponsored esports athletes playing League of Legends to become micro-influencers to drive people 18 – 24 years to “find their words.” The goal is to help the followers address their mental health needs and break the stigma.
2. Let’s Dance
Cynthia Marshall, CEO of the Dallas Mavericks, had the audience speaking to their neighbors and dancing the Cupid Shuffle. The multi-effort to engage proved her point that leadership requires intention, insight, and inclusion. She created an inclusive dance party where the audience learned or taught the Cupid Shuffle. She reminded us that diversity is about the mix, but inclusion is what you do once you are there. Or simply put, diversity is being invited to the party, but inclusion is being asked to dance. Finally, she taught us that a leader should take action, take time to celebrate, and speak the truth. She clearly described herself and that session.
3. CCBHCs
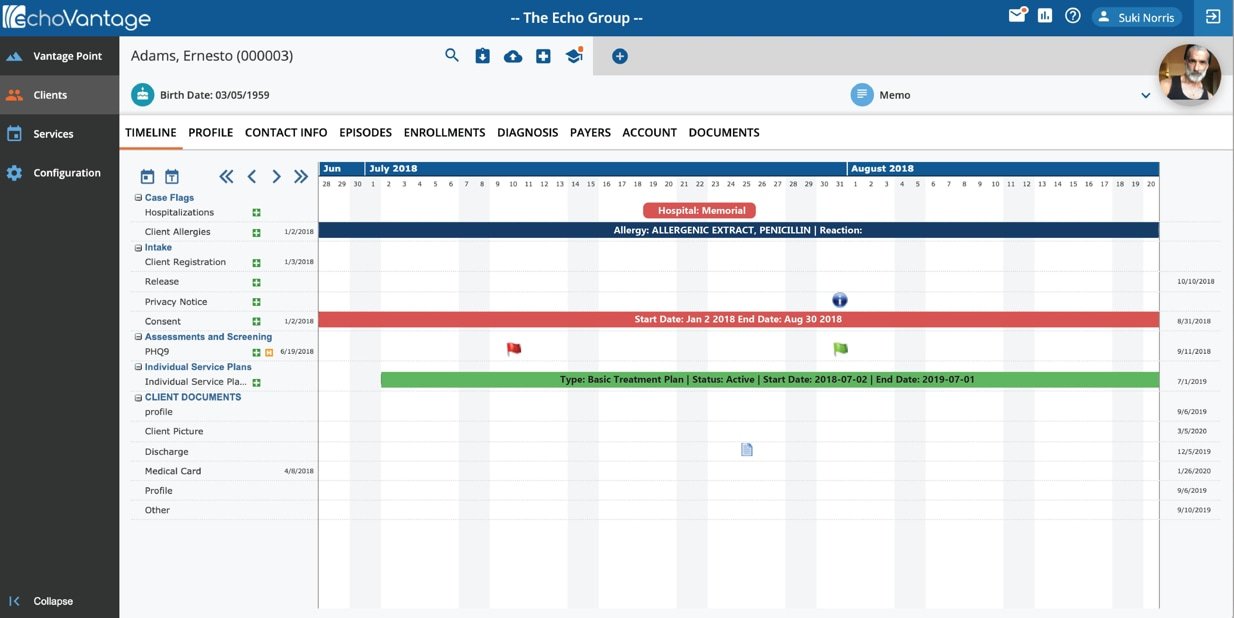
While these issues are important, much of the focus was on CCBHCs, outcome measures, and value-based payment. CCBHCs are in all but seven states and two territories. The National Council for Wellbeing estimates that CCBHCs serve 1.5 million people, which continues to grow. What does that mean? 1.5 million people have expanded access to care, with decreasing wait times. Crisis services are available, and there is improved collaboration with criminal justice. Finally, CCBHCs are working to address health disparities. The work of CCBHCs requires an EHR that understands the unique needs, from flexible treatment functionality to real-time dashboards that provide insight into the quality of care for the patient and the agency as a whole.
4. Outcomes
Many sessions addressed outcomes to improve treatment to support new payment methodologies. In support of treatment, outcomes help define the use of evidence-based practice. The goal is to utilize the data in the system to improve treatment on an ongoing basis. Outcomes are not just on dashboards but are now part of the clinical treatment. Outcomes are updated based on the treatment provided, and the current level of care related to the treatment plan is visible as you provide care. Without searching through the record, you know what to work on and where the client needs help. Outcomes are no longer an indication of how you did but are now indicators of how you are doing.
5. Value-Based Payment
Value-based payment (VBP) is not only a CCBHC requirement but is expanding to Medicaid throughout the country. Value-based payments are a challenge to many mental health agencies as payment focuses on quality and care costs. The ability to translate this payment structure to behavioral health has been challenging. Many mental health agencies had not prepared to manage the risk that VBP incorporates into the payment structure. The VBP focus is on outcomes and cost-effective care. The new norm is to focus on treatment methodologies, on-demand dashboards, and flexible billing functions.
6. 988 is Coming
Another session discussed the 988 system. I had a bit of an advantage because I was lucky enough to sit on the plane with someone implementing a 988 system and setting up to be the call and referral center. We know the 988 system is complex, but when it is nationwide, we will be able to use the data to improve the system and better coordinate care on an ongoing basis.
The new 988 number is a universal telephone number in the United States for the purpose of national suicide prevention and mental health hotline. SAMSHA estimates that by 2023 the 988 lines will receive 4.2 Million calls and 3.4 Million chats. The five-year vision includes that 90% of calls will be answered in the state by 2023; by 2025, 80% of callers will have access to rapid crisis response, and by 2027 80% of callers will have access to community-based crisis centers.
7. Population Health
Population health nicely wraps up each of the previously discussed areas. The first goal of population health is to use data to inform programs, prevent or intervene at the earliest moment, and intervene at the population level. You also have to consider the whole person, not just the behavioral health needs, but the physical health needs and the social intervention needs of the person and the population. As a result of the population health focus, mental health agencies must consider integrated care to ensure that their clients receive physical health care as part of their treatment. Integrated care may result from CCBHCs or Behavioral Health Homes, or agencies developing relationships with PCPs. Population health includes the continuum of care for the individuals that create the population.
8. Brain Health
Two persons from the McKinsey Health Institute spoke about brain health in a general session. Brain health includes positive mental health and the full range of mental, substance use, and neurological conditions. Brain health is a critical determinant of overall health. The focus of brain health is more than the absence of disease; it is the state of determining your abilities, notwithstanding the challenges of everyday life. By addressing brain health worldwide, McKinsey Health Institute posits we could add 45 Billion extra years of higher quality life, roughly six years per person on average. On that note, I spent the balance of NatCon thinking about how I might use my six years.