Breaking News: The Echo Group Acquired by Therapy Brands Read More
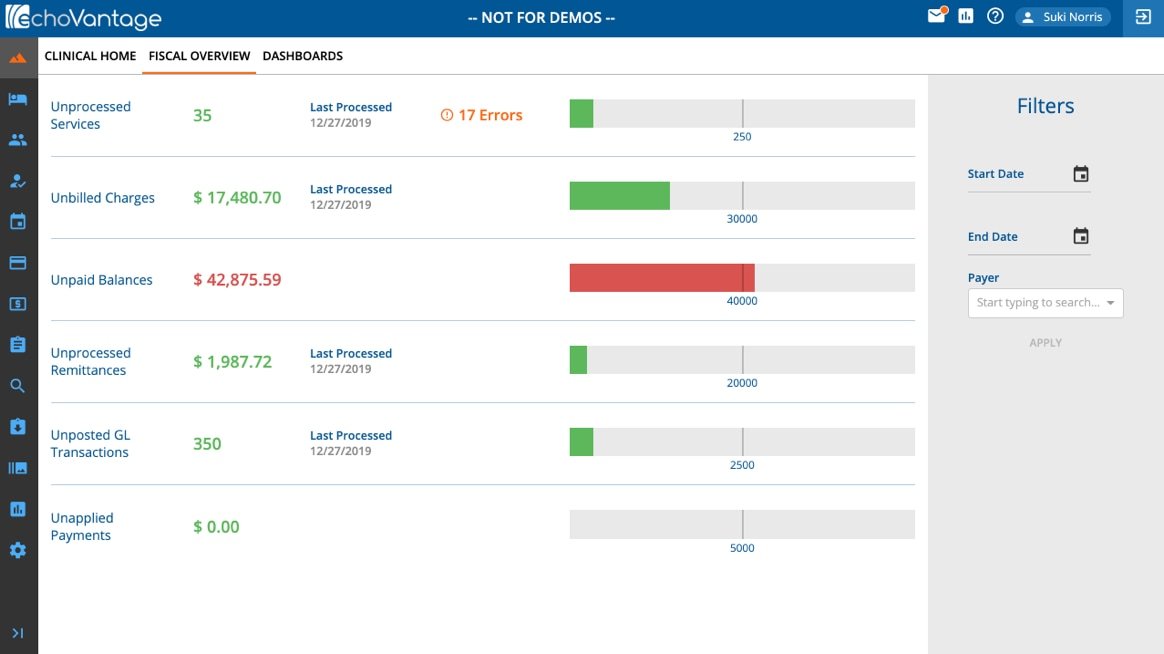
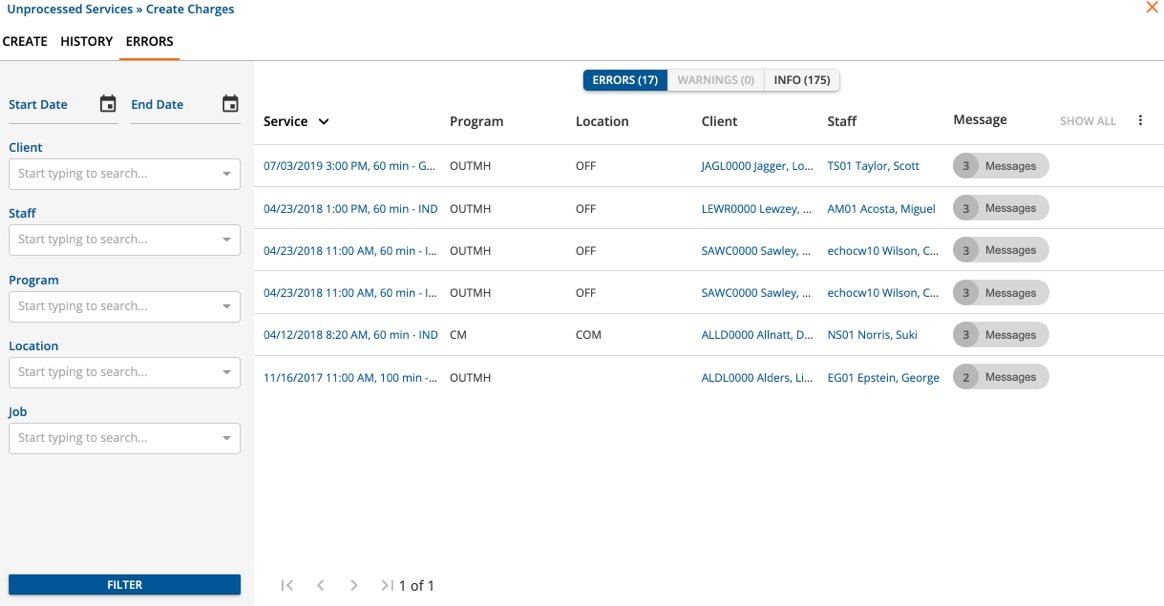
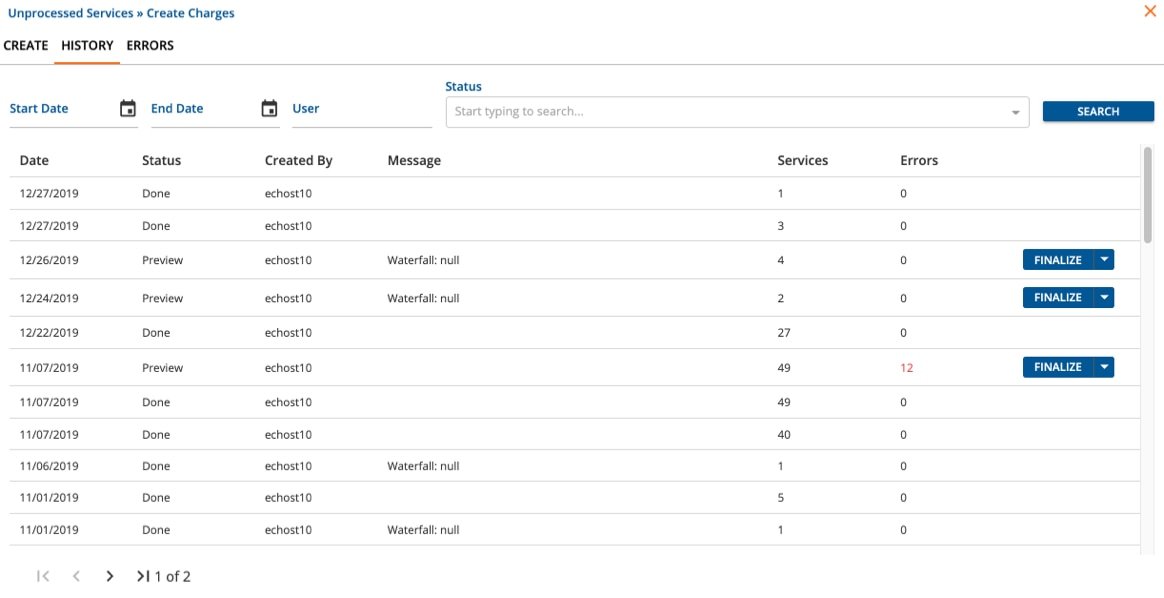
Let us handle your billing so that you can focus on managing. Our team handles:
Increased Collection Rate
Reduction Outstanding Receivables
Months Result Time
We review the denials and resolve or work with you to resolve depending on the nature of the denial.
We can work with you to determine the best mix of payers to assign to RCM.
Of course, you can review the billing information at any time of the month. You can also reach out to your RCM team to answer any questions as they arise.